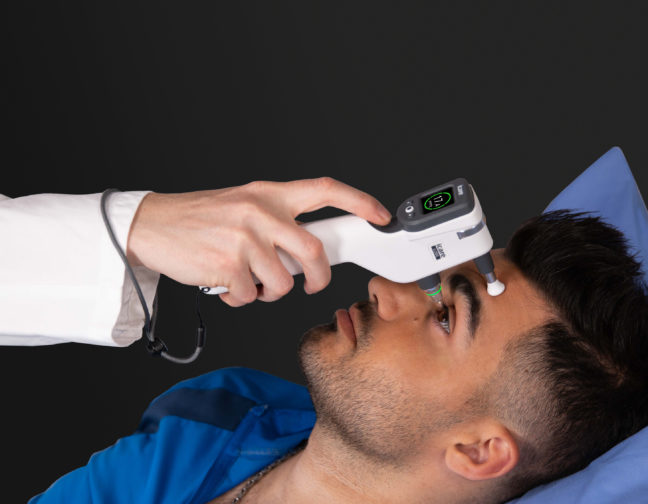
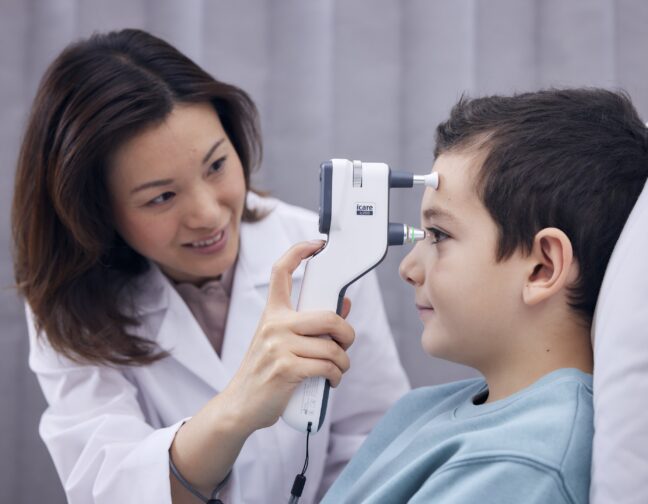
Comprehensive diurnal IOP profiles are key in ensuring that glaucoma patients receive the most appropriate care. According to recent research, the iCare HOME self-tonometer demonstrates the ability to characterize diurnal IOP patterns accurately within one week of using the device – making it a highly useful tool for modern glaucoma management.
A recent study by Tong et al.¹ highlights that diurnal IOP profiles obtained using the iCare HOME self-tonometer may reflect IOP responses to treatment more accurately than standard IOP measurements in the office. This more comprehensive understanding of IOP fluctuations offers the eye care professional valuable support in making glaucoma treatment decisions.
The study investigated daily peak IOPs, IOP fluctuations, and mean IOPs in patients with glaucoma and ocular hypertension using latanoprost and timolol. The effects of the medications were assessed by comparing mean percentage IOP reductions.
Current IOP measurement practices may fall short of the goal of evaluating therapy consistently and accurately
IOP measurement remains a fundamental component in the diagnosis and monitoring of glaucoma. However, current practices rely on single in-office measurements as the basis for choosing the appropriate treatment strategy.
According to Tong et al., IOP information recorded in this snapshot style solely during office hours does not show short-term IOP fluctuations and may fail to portray IOP peaks. Previous research shows that peak IOP measurements fall outside of office hours in up to 79% of glaucoma patients. 2–4
This clearly indicates that in-office measurements alone do not suffice to reflect diurnal IOP profiles adequately.
Comprehensive diurnal IOP profiles obtained via self-tonometry can help eye care professionals to optimize treatment decisions
Tong et al. conclude that a more comprehensive characterization of diurnal IOP patterns is key in ensuring that glaucoma patients with slow disease progression receive the best possible care. The study emphasizes the clinical potential of new technologies that enable IOP measurement outside office hours, including self-tonometry devices such as the iCare HOME rebound tonometer.
In the crossover treatment trial, 14 participants took self-measurements of IOP with the iCare HOME tonometer four times a day for 1–4 weeks, depending on which medication program they were on. IOP fluctuations reached a target reduction of 30% more frequently than peak and mean IOPs did on both latanoprost and timolol.
The study found that the analysis of IOP fluctuation measured with self-tonometry was more consistent in evaluating target IOP, which highlights the importance of diurnal IOP profiles in ascertaining IOP responses to topical therapies. These findings also demonstrate that the iCare HOME tonometer can characterize IOP variations appropriately and be of significant use in clinical decision making.
The iCare HOME tonometer can characterize diurnal IOP patterns accurately within one week of self-tonometry
According to the treatment trial, one week of using the iCare HOME self-tonometer is sufficient to reliably portray diurnal IOP profiles. Furthermore, several previous studies show that at least 75% of patients can successfully learn to perform self-tonometry using the iCare HOME. 5–7
This clinically promising figure is based on research on the world’s first self-tonometer, the iCare HOME tonometer. Its successor, the iCare HOME2 tonometer is even easier to use, comes with intuitive training materials, and can measure IOP in both sitting and supine positions.
Tong et al. recognize that the option of self-tonometry in the supine position could be invaluable in investigating differences between medications in more detail.
¹ Tong J., Huang J., Kalloniatis M., Coroneo M., Zangerl B. Clinical Trial: Diurnal IOP Fluctuations in Glaucoma Using Latanoprost and Timolol with Self-Tonometry. Optometry and Vision Science: August 2021 – Volume 98 – Issue 8 – p 901-913. doi: 10.1097/OPX.0000000000001751
2 Barkana Y, Anis S, Liebmann J, et al. Clinical Utility of Intraocular Pressure Monitoring Outside of Normal Office Hours in Patients with Glaucoma. Arch Ophthalmol 2006;124:793–7.
3 Konstas AG, Mantziris DA, Cate EA, et al. Effect of Timolol on the Diurnal Intraocular Pressure in Exfoliation and Primary Open-angle Glaucoma. Arch Ophthalmol 1997;115:975–9.
4 Hughes E, Spry P, Diamond J. 24-Hour Monitoring of Intraocular Pressure in Glaucoma Management: A Retrospective Review. J Glaucoma 2003;12:232–6.
5 Huang J, Katalinic P, KalloniatisM, et al. Diurnal Intraocular Pressure Fluctuations with Self-tonometry in Glaucoma Patients and Suspects: A Clinical Trial. Optom Vis Sci 2018;95:88–95.
6 Chen E, Querat L, Akerstedt C. Self-tonometry as a Complement in the Investigation of Glaucoma Patients. Acta Ophthalmol 2016;94:788–92.
7 Mudie LI, LaBarre S, Varadaraj V, et al. The iCare HOME (Ta022) Study: Performance of an Intraocular Pressure Measuring Device for Self-tonometry by Glaucoma Patients. Ophthalmology 2016;123:1675–84.