Originally published by Ophthalmology Times Europe
By Kaweh Mansouri, MD
Visual field testing to identify functional damage is an essential component of the diagnostic evaluation for glaucoma detection and monitoring. Full threshold testing with automated perimetry is the gold standard for identifying and quantifying glaucoma-related functional damage and can be done using different perimeters that are based on various technologies.
Combining perimetry, fixation loss correction, and confocal TrueColor fundus imaging with patient- and technician-friendly features, the COMPASS Automated Perimeter with active Retinal Tracking (Centervue Spa, a company of iCare Finland Oy; Vantaa, Finland) is a unique tool that takes visual field testing and interpretation to a higher level.
iCare COMPASS functions and features
Visual field testing
Automated perimetry with COMPASS is fully compatible with standard 24-2, 30-2 and 10-2 visual field testing containing age-matched databases of retinal sensitivity in normal subjects. In addition, COMPASS offers SupraThreshold and Quick SupraThreshold testing for rapid visual field loss screening. Done using the standard 24-2 test grid, the SupraThreshold test takes approximately 2 to 3 minutes per eye. The Quick SupraThreshold test using an optimally reduced 24-2 grid is even faster, taking just 30 to 90 seconds per eye and allowing testing of both eyes sequentially using the “OU” option.
Visual field testing with COMPASS is done using Active Retinal Tracking. During the examination, continuous and automated tracking of eye movements by infrared scanning of the retina provides real-time compensation for fixation losses and assures that the stimulus position is correct. Perimetric stimuli are automatically repositioned prior to and during projection based on the current eye position. Stimuli lost due to blinking are automatically repeated and do not interrupt the test.
TrueColor confocal imaging
COMPASS generates 60° confocal images of the retina in three modalities: TrueColor, infrared and red-free. By combining a confocal engine with a white light LED source to illuminate the retina, COMPASS generates fundus images that are sharp, high contrast, and natural in colour. High quality images are obtained even in eyes with media opacity because of the confocal technology. Registration between the retinal image and retinal sensitivity threshold allows a direct correlation between visual function and retinal anatomy.
My clinical perspective
Visual field testing and acquiring high resolution, true colour images of the fundus and optic nerve head are essential when evaluating patients with glaucoma. Not only does COMPASS address both needs in a single time-saving examination, but it also generates a superimposed image that shows a precise overlap between areas of depressed sensitivity and areas of the retina with indications or source of defects, some of which cannot be seen with optical coherence tomography only.
The opportunity to simultaneously perform perimetry testing and fundus imaging is by itself a great benefit of COMPASS compared to standard automated perimeters, but its active retinal tracker further distinguishes COMPASS from standard automated perimeters that cannot actively compensate for eye movements during testing. The retinal tracking technology serves to increase test precision by measuring sensitivity at specific retinal locations with high topographic accuracy. Thus, it ensures accurate correlation between function (i.e. retinal threshold values) and structure (retinal appearance) and decreases test-retest variability. I believe that active retinal tracking brings added value for improving the clinical accuracy of visual field tests, their interpretation in general and especially in eyes that have several pathologies at different stages, and the reliability of detecting glaucomatous progression.
In addition, because active retinal tracking automatically positions stimuli correctly on the retina, despite fixation losses, blinking or movements of the eye or head, and since lost stimuli are repeated automatically, patients can blink, close the eye, or rest and continue without loss of data and technician involvement during COMPASS visual field testing. This decreases stress and fatigue in patients, is convenient for the operator, and decreases the need for retakes due to unstable fixation.
Multiple other features of the COMPASS make visual field testing operator-friendly, easier for patients, and more efficient. Designed with auto-focus that compensates for spherical refractive errors between -12 D and +15 D, COMPASS avoids the need for using trial lenses to perform visual field testing. Auto-focus therefore eliminates the potential for lens rim artefacts that can result in test misinterpretation and also saves time.
Further enhancing workflow efficiency, visual field testing with the iCare COMPASS is done without mydriasis for pupils larger than 3mm. Consequently, there is no delay waiting for the pupil to dilate nor any need to wait for the eye to adjust after a flash of light. As another time-saving feature, cleaning of the COMPASS is quick and simple because it has a smooth, narrow, convex design, lacks any sensitive structures, like a bowl, and has no trial lens assembly. The machine’s surfaces can be easily disinfected using only an alcohol wipe. This ease of decontamination holds increased importance because of COVID-19. All of these contributors to efficiency more than compensate for the slightly increased duration of combined visual field testing/fundus imaging with COMPASS compared to standard automated perimeters.
Clinical case
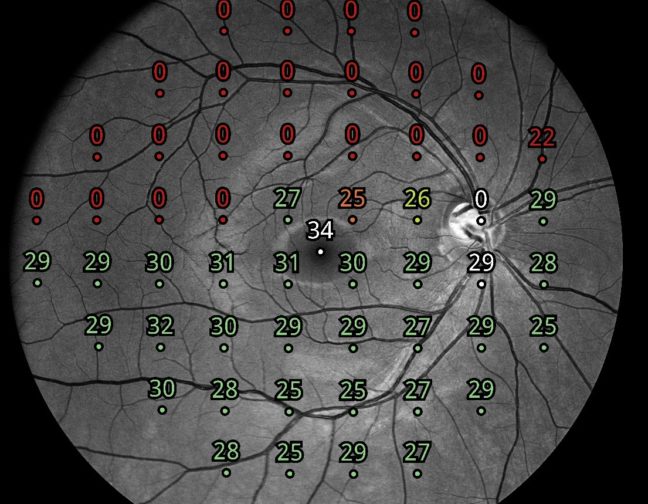
Figures 1 and 2 show the COMPASS printout and fundus image from one of my patients. The fixation plot in the printout (bottom left) shows that the patient had unstable fixation, but even in this situation it was possible to obtain a reliable visual field with adequate false positive and false negative indices as well as an MD of -2.68. The COMPASS fundus image revealed a significant peripapillary atrophy (as shown in the red-free image and in the zoomed ONH colour image) that is well represented as an enlarged blind spot on the visual field. The printout also shows a single focus in the superonasal visual field that needs to be confirmed by repeat testing. By providing excellent visual field test repeatability, COMPASS will enable the determination of whether the defect is an artefact or represents an early sign of glaucomatous damage.
Conclusion
I find that COMPASS brings many benefits to clinical practice. It is the first automated perimeter that can perform standard visual field tests using a real-time retinal tracker while simultaneously delivering ultra-high resolution confocal TrueColor fundus images. In addition, it saves time in many ways and makes visual field testing more patient- and technician-friendly for many reasons.
In a study where patients underwent perimetric evaluation with both the Humphrey Field Analyzer and COMPASS, results of a post-test interview showed the participants had a strong preference for the COMPASS examination.1 Importantly, our own technicians give very positive feedback about their experience with this unique diagnostic device. Finally, I give COMPASS high ratings as a clinician because with its capabilities and benefits, COMPASS enables me to optimize patient care by helping me detect glaucoma and its progression accurately and early.
Dr. Mansouri is a consultant ophthalmologist, Clinique de Montchoisi, Lausanne, Switzerland, and adjoint professor, Department of Ophthalmology, University of Colorado Anschutz Medical Campus, Denver, Colorado. Dr. Mansouri is a consultant to iCare. CENTERVUE S.P.A., ICARE FINLAND OY are parts of REVENIO GROUP and represent the brand iCare.
REFERENCE
1. Morbio R, Longo C, De Vitto AML, Comacchio F, Della Porta LB, Marchini G. Comparison between Fundus Automated Perimetry and Humphrey Field Analyzer: Performance and usability of the Fundus Automated Perimetry and Humphrey Field Analyzer in healthy, ocular hypertensive, and glaucomatous patients. Eur J Ophthalmol. 2021;31(4):1850-1856.